Introduction to BRCA, Hereditary Risk & Reconstruction
Prophylactic mastectomy doesn’t limit your reconstructive choices. It gives you the opportunity to plan reconstruction at the same time or after healing.
Carrying a BRCA1 or BRCA2 gene mutation, or having a strong family history of breast cancer, can make prophylactic mastectomy a proactive and deeply personal choice.
If you’re considering surgery to reduce your cancer risk, understanding your reconstruction options is an essential part of planning ahead.
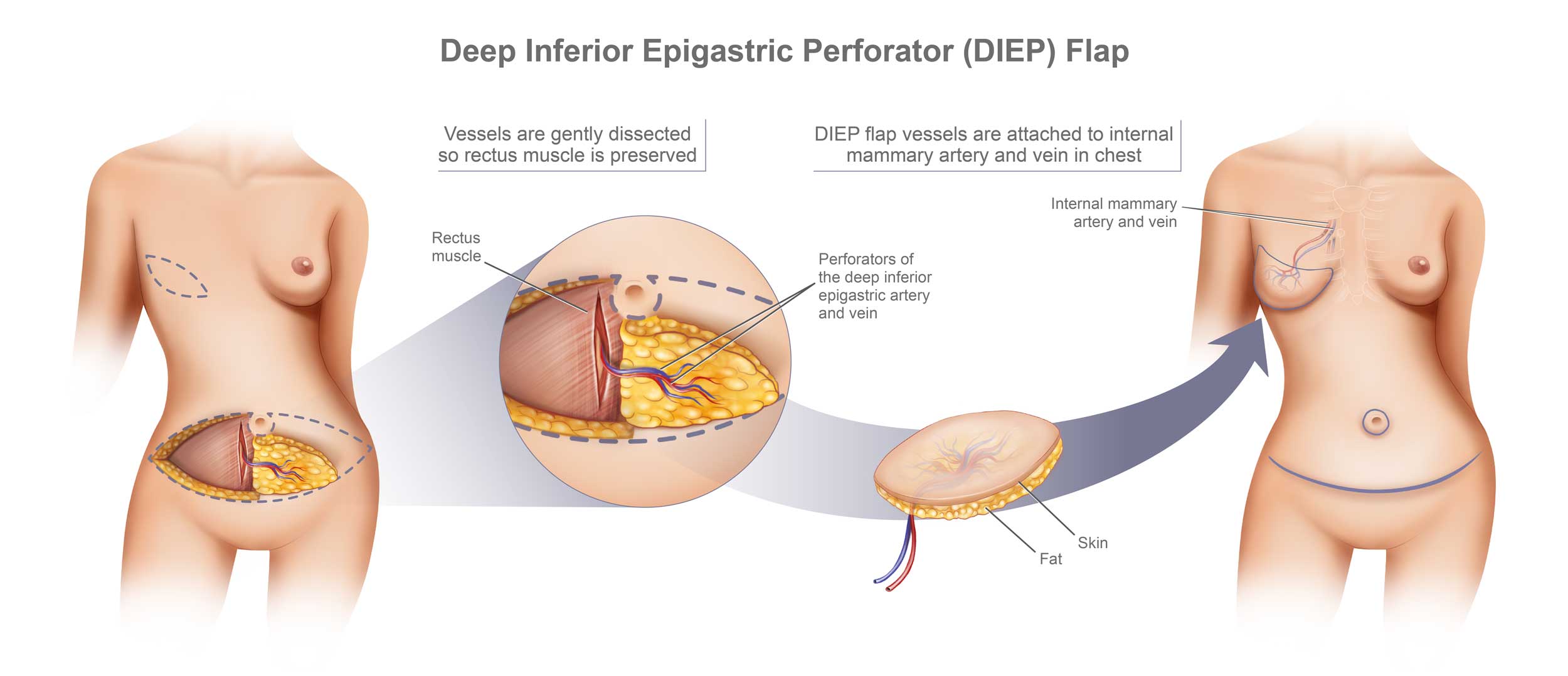
Autologous reconstruction replaces breast tissue removed during prophylactic mastectomy with your own natural tissue—often from the abdomen—to recreate full, symmetrical breasts without sacrificing muscle. This “like-for-like” approach offers the most natural foundation for women undergoing surgery due to BRCA or hereditary cancer risk.
Under the advanced microsurgical expertise of Dr. Joshua L. Levine, a world-renowned specialist in natural tissue breast reconstruction, all women undergoing prophylactic mastectomy are candidates for autologous reconstruction.
Your Path Forward – What You’ll Learn Here:
We cover the following 4 sections to walk you through where you currently may be, what your options are, what you can expect, and how to move forward.
Part 1

Your current experience
Causes and Symptoms
How Hereditary Risk Shapes Your Starting Point
Understanding your genetic risk helps guide your decisions about mastectomy, timing, and the type of reconstruction that will support your long-term health and peace of mind.
If you’ve recently learned you carry a BRCA or other hereditary gene mutation, you may be processing what this means for your future and exploring whether prophylactic mastectomy is the right next step.
This is a moment of careful consideration, balancing risk, family history, and your desire for peace of mind moving forward. Knowing your starting point helps clarify your options and gives you a stronger sense of direction as you begin planning reconstruction.
What Shapes Your Reconstruction Plan:
Understanding your BRCA or hereditary mutation helps clarify why risk-reducing mastectomy is often recommended.
These gene changes can significantly increase lifetime breast cancer risk, even at younger ages.
Knowing this risk gives you the information you need to make a proactive, empowered decision about surgery and reconstruction.
Prophylactic mastectomy can be planned on your timeline, giving you the opportunity to choose the technique and timing that best fit your goals.
Your surgeon will discuss nipple-sparing options, skin-sparing approaches, and how the procedure supports long-term cancer prevention.
This step forms the surgical foundation that reconstruction will build upon.
After mastectomy, you can choose natural tissue (autologous) reconstruction to create soft, long-lasting, implant-free results.
These options use your own tissue to rebuild breasts that feel natural and age with your body.
Understanding these methods early helps you plan reconstruction with confidence and clarity.
Part 2

Your Empowered Choice
Corrective Autologous Procedures
Understanding Autologous Reconstruction with Prophylactic Mastectomy
Because prophylactic mastectomy removes most or all breast tissue to reduce cancer risk, autologous reconstruction offers the most natural, long-lasting way to restore softness, contour, and balance, without implants or future implant replacement.
Because prophylactic mastectomy removes most or all breast tissue to reduce cancer risk, autologous reconstruction offers the most natural, long-lasting way to restore softness, contour, and balance—without implants or future device replacement.
Part 3

Your Future, Blossoming
Comfort, Look, Feel, and Long-Term Results
How Your Life Improves After Preventative Mastectomy and Reconstruction
Autologous reconstruction after prophylactic mastectomy offers a stable, natural way to restore breast shape while reducing long-term cancer risk.
This section explains what this reconstruction provides and how to choose the timing that aligns best with your medical needs, lifestyle, and readiness.
Timing Options
The three options below help you understand when reconstruction can safely take place and what each approach means for your recovery and long-term results.
Reconstruction is performed in the same operation as your prophylactic mastectomy.
This allows you to wake up with breast shape already restored and minimizes the number of surgeries required.
Many patients choose this approach for convenience and emotional continuity. There is no period of having a flat chest.
It is safe, efficient, and often provides the smoothest overall recovery.
Staged-immediate reconstruction happens shortly after mastectomy, typically within days to a few weeks.
This timeline is useful if additional planning, coordination with breast surgeons, or short healing time is needed before reconstruction.
It maintains most of the advantages of immediate reconstruction while giving your team more flexibility.
The final results remain just as natural and long-lasting.
Delayed reconstruction happens months or even years after prophylactic mastectomy.
Some women prefer this approach to focus first on risk reduction, life events, or personal readiness.
Even with a delay, autologous reconstruction still provides soft, natural, and symmetrical results using your own tissue.
This option keeps all reconstruction possibilities open and can be pursued any time you feel prepared.
Part 4

Your Surgical Path Forward
Reach Out With Questions
Meet Microsurgeon, Dr. Joshua L. Levine:
Patient Testimonials and Results
Real experiences can be incredibly reassuring for women navigating hereditary breast-cancer risk and the decision to undergo prophylactic mastectomy. Many of Dr. Levine’s patients arrive seeking reliable, natural options and want to understand what life can look like after reconstruction.
Their stories reveal what becomes achievable with advanced autologous reconstruction. Below are insights into what patients consistently share about their outcomes.
Dr. Levine’s Patient Testimonials
View Dr. Levine’s Patient & Results
The photographs in this section are of actual patients of Dr. Joshua Levine. They have undergone various types of natural tissue breast reconstruction (perforator free flaps), i.e. DIEP/SIEA, PAP, GAP, delayed, immediate, with nipple-sparing mastectomy, etc.
Dr. Joshua L. Levine, MD, FACS
World-Renowned Natural Tissue Breast Reconstruction Surgeon
Dr. Joshua Levine is a world-renowned perforator flap breast reconstruction surgeon. Meaning, all of his breast reconstruction procedures, are muscle-sparing, using only your own natural tissue to restore your breast(s).
With his advanced techniques, such as stacked combination flaps, or utilizing the delay phenomenon in staged-immediate reconstruction, all women, no matter how thin and no matter what body type, are candidates for natural tissue, muscle-sparing, implant-free breast reconstruction.
As Seen On: US News & World Report, sharecare.com, diepflap.com
Plan Your Next Steps and Reach Out
If you’re experiencing discomfort, dissatisfaction, or long-term issues from a previous reconstruction, reach out today. We are here to provide you with thoughtful, individualized guidance based on your unique history, anatomy, and goals.