When Choosing Between Breast Implants vs Natural Reconstruction, Your Surgeon’s Expertise Makes a Difference.
Dr. Joshua Levine is a world-renowned perforator flap breast reconstruction surgeon. Meaning, all of his breast reconstruction procedures, are muscle-sparing, using only your own natural tissue to restore your breast(s).
With his advanced techniques, such as stacked combination flaps, or utilizing the delay phenomenon in staged-immediate reconstruction, all women, no matter how thin and no matter what body type, are candidates for natural tissue, muscle-sparing, implant-free breast reconstruction.
While utlizing implants for reconstruction requires less operating time in the OR than natural tissue perforator flap reconstruction, implants have risks associated with them, as well as don’t provide the same patient results that return a woman’s breasts to their natural look, feel, and touch.
FDA.gov:
Breast Implant Safety Requirements
New York Times Article:
Breast Cancer May Be Linked To Additional Cancers, F.D.A Warns
Comparing:
Breast Reconstruction with
Implants vs. Natural Tissue (Autologous)
Risks of Breast Implant Complications
Breast cancer radiation and chemotherapy significantly increase risks, complications, and pain for women opting for implant breast reconstruction.
Benefits of Natural Reconstruction
When breast cancer survivors have undergone chemotherapy or radiation, choosing natural reconstruction over breast implants can often be the safer option.
Patient’s Seeking Implant Failure Corrective Surgery Have Shared The Following Sentiments with Dr. Levine.
“Stress balls. Feels like a brick. Lead things on my chest. Vulnerable, always aware.”
“No day goes by ever ever ever that I’m not uncomfortable.”
“Imagine living every day with an acorn stuck under your tongue, and you can’t get it out.”
“Feels loose. Pain like something scratching, something has come loose.”
“Never have been pleased cosmetically. Not the slightest bit symmetrical.”
“I don’t want to have any pain. Feels like a rock. Looks horrible. Strangled. Skin looks like mush.”
“Feels like someone’s twisting it back and forth.”
“Ice cold. Constant pressure.”
“Can’t do yoga. Can’t jog. Can’t Sleep. Can’t wear a bra.”
“Don’t look like breasts. Just two half cantaloupes.”
” Popping when working out. Can’t do pull-ups. Always in discomfort.”
“Feels tight, like two glasses or two bowls pressed up against me. Numbness.”
Candidacy:
Procedure Options for
Implants vs. Natural Tissue
Reconstruction
Advanced Autologous Techniques
Not all surgeons are able to provide advanced breast reconstruction techniques. Therefore they may recommend implants or flap procedures that require muscle sacrifice when in fact you may be a candidate for true, muscle-sparing natural tissue breast reconstruction.
The Surgical Delay Phenomenon | Breast Implants vs. Natural Breast Reconstruction
What we know from many years of experiments and studies that have been done over decades, is that when cutting off part of a blood supply to a certain area, the blood vessels that remain, become larger and more robust, in order to continue to supply to that tissue. This is called the delay phenomenon.
When we think about this concept as it relates to the abdomen, it means that if we are going to transfer a certain amount of tissue from the abdomen based on one blood vessel, as we do in the DEIP, we may be limited in the amount of tissue or tissue volume that one blood vessel supplies.
If we are strategic about the way we make our surgical delay incision and very thoughtful about the way that we remove certain blood vessels, we can select the blood vessel and train it to supply the tissue that we want.
In the last few years, we’ve found we are able to convert patients who would not ordinarily have been candidates for the use of their abdomen in breast reconstruction, into abdominal flap candidates.
Timing The Surgical Delay Procedure:
About a week prior to abdominal flap transfer, we surgically remove the blood supply to areas of the abdominal tissue that will be transferred, and strategically leave the one blood vessel we’d like to use for the flap. This allows that one blood vessel to grow in size as it “learns” to profuse the additional tissue volume where the blood supply has been diminished. This is called the delay phenomenon or surgical delay.
Because of the power of this new technique called the surgical delay as it applies to abdominal flaps, we have found it to be an extremely useful and powerful adjunct to routine abdominal flap procedure.
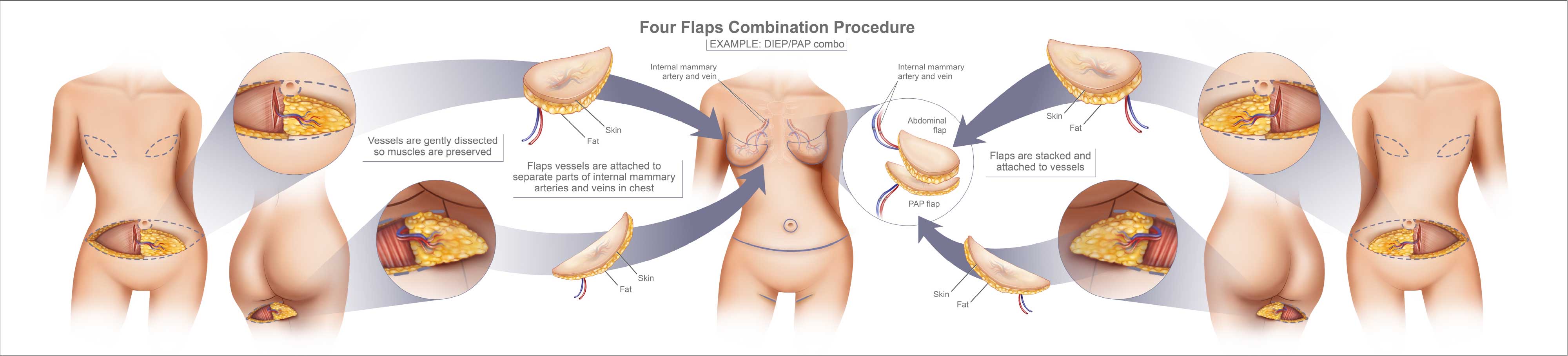
Advanced Procedure Stacked Combination Flap | Breast Implants vs. Natural Breast Reconstruction
All women are candidates for autologous breast reconstruction. Even very thin women can use their own body tissue to reconstruct both breasts. When a patient has scant extra body fat, it is sometimes appropriate to use tissue from more than one donor site. These procedures are called “stacked” or “combination” flap reconstructions.
The most common “stacked” flap is from the abdomen. In unilateral breast reconstruction, we use both halve of the to create one breast reconstruction
When a bilateral breast reconstruction is done for a thin woman, four flaps may be recommended. This would usually include one half of the abdomen (hemi-abdomen) PLUS another flap such as a PAP flap for each breast.
Chemo Radiation Implant Risks | Breast Implants vs. Natural Breast Reconstruction
When breast implants are placed after radiation therapy, there is an increased incidence of aesthetic and physical issues that arise.
Potential problems can include severe hardening of scar tissue around the implant, chest wall discomfort, changes in implant position, and even implant loss.
Radiation cancer treatment can have an undesirable impact on the tissue surrounding an implant.
The body considers a breast implant a foreign object and isolates it with a barrier of protective scar tissue. This tissue, known as a capsule, is usually soft and unnoticeable. However, chest wall radiation increases the chance that the tissue capsule will harden and contract around an implant, creating a breast that is frequently tight, high in position, hard, and uncomfortable. This is a condition known as capsular contracture.
Prior radiation to the chest wall can also create unique challenges for implant-based reconstruction in the future. For example, radiation permanently adversely affects skin and underlying tissue quality. As a result, the risk of complications and poor aesthetic outcome are significantly increased.